Dynamics of the psychological features and clinical symptoms in mitral valve prolapse patients receiving long-term integrative psychotherapy for anxiety disorders
Abstract
The purpose of the study was to investigate the dynamics of the psychological features and clinical symptoms in mitral valve prolapse (MVP) patients receiving long-term integrative psychotherapy for anxiety disorders (AD) and to investigate the psychological factors of their improvement in mental health as a result of psychotherapy. Thirty-two MVP patients with AD attended long-term integrative psychotherapy. Psychological and clinical examinations of the patients were made before and after the therapy courses and in a follow-up study after 2, 5, and 10 years. Data from the study show that 78.1% of the patients who attended psychotherapy sessions demonstrated valid improvements in self-rated psychological well-being and a reduction in their anxiety levels. Analysis of emotion-regulation strategies showed that psychotherapy encouraged the use of strategies effective for solving adaptive tasks. Positive dynamics in the development of personality reflection, the recognition of one’s emotional experiences, improved skills of self-regulation, and growing awareness of actual needs, individual purposes, and personality resources—all were associated with the reduction of MVP clinical symptoms. The psychiatrist who interviewed the patients reported that most of them were in sustained remission.
Received: 27.06.2014
Accepted: 30.08.2014
Themes: Clinical psychology
PDF: http://psychologyinrussia.com/volumes/pdf/2014_3/2014_3_66-79.Pdf
Pages: 66-79
DOI: 10.11621/pir.2014.0306
Keywords: long-term integrative psychotherapy, emotion regulation, personality reflection, self-regulation, mitral valve prolapse (MVP), anxiety disorders (AD), quality of life (QOL), psychological well-being
Our research interest in mitral valve prolapse (MVP) patients is far from being accidental. MVP is widespread, affecting between 30.8% and 42.0% of the population (Barlett, Kirtley, & Mangham, 1991; Devereux, Kramer-Fox, & Kligfield, 1989; Scordo, 2007; Stefanadis, & Toutouzas, 2000).
Researchers note a pronounced dissociation between numerous subjective complaints of the patients, on the one hand, and the scanty data from objective studies, on the other (Joiner & Cornman, 1986; Scordo, 2007); they also present indications of widespread anxiety disorders (AD) accompanying MVP and the unpleasant inclusion of the formation of “functional MVP” within panic disorder (some authors assert that panic attacks not only may be “triggered” by MVP but may lead to its development: Coplan, Papp, King, & Gorman, 1992; Gorman et al., 1988). There are cases of a significant reduction in the intensity of clinical symptoms after psychotherapy and antidepressant or anxiolytic treatment (Gonzalez et al., 2002; Pariser, Reynolds, Falko, Jones, & Mencer, 1981; Scordo, 2007; Stavrakaki, Williams, Boisjoli, Vlad, & Chasse, 1991); there is even some evidence that such treatment may be symptomatolytic—that is, it may result in the complete disappearance of echo-cardio-graphic MVP indicators in patients suffering from panic disorders (Coplan et al., 1992).
Research objectives
The purpose of the study was to investigate the dynamics of psychological features and clinical symptoms in MVP patients with AD receiving long-term integrative psychotherapy and to investigate the psychological factors of their improvement in mental health as a result of psychotherapy.
Research design
Thirty-two MVP patients with AD attended integrative psychotherapy on request (1 to 2 sessions per week, individual assessments). Among them 18 (56.3%) received psychotherapy in addition to Alprazolam medication (with a fixed dose 1.5 to 4.5 mg per day, with dose titration if necessary depending on the severity of the AD, within periodical treatment).
The therapy courses were conducted from 1997 to 2012. The duration of the psychotherapy ranged from 5 months to 2 years. The age of the patients during therapy ranged from 25 to 37 years. Most of the patients were women (28 people; 87.5%).
Psychological and clinical examinations of the patients were conducted before and after the therapy courses; the follow-up study was undertaken after 2, 5, and 10 years.
The types of AD and their frequency in the MVP patients are presented in Table 1.
Table 1. AD in patients with MVP before therapy
Disorders |
Percentage of patients (%) |
Panic disorder without agoraphobia |
28.1 |
Panic disorder with agoraphobia |
25.0 |
Generalized anxiety disorder |
46.9 |
Research methods
Psychological testing embraced assessment of the following indicators:
- Anxiety level was assessed on the Spielberger State-Trait Anxiety Inventory (STAI) (Spielberger, Gorsuch, Lushene, Vagg, & Jacobs, 1983).
- Quality-of-life (QOL) indicators were assessed through the Visual Analog Scale (VAS) (the “well-being” dimension); the Disability Scale (DISS) (the dimensions of “work,” “social life,” and “personal life”) (Sheehan, 1983); and the Ryff Scales of Psychological Well-Being (PWB) (Ryff, 1989; Ryff, & Keyes, 1995).
- The study of emotional experiences and emotion regulation employed our modified version of the Rosenzweig Picture Frustration test (Rosenzweig, 1978; Zinchenko & Pervichko, 2012).
The medical part of the study involved a complex of procedures aimed at establishing a diagnosis for each patient (all patients had an ultrasonic cardiogram) and at assessing the degree of intensity of MVP clinical symptoms and signs (MVP level, intensity of symptoms in the dysautonomic nervous system, frequency and intensity of vascular disorders, and so forth).
An assessment of psychopathological status and its dynamics was conducted using data from a psychiatric examination conducted in accordance with ICD-10 procedure-coding criteria, from the Clinical Global Impression Scale (Guy, 1976), and from the Marks-Sheehan Phobia Scale and the Sheehan Panic and Anticipatory Anxiety Scale (Sheehan,1983; Sheehan & Harnett-Sheehan, 1990).
Statistical analysis consisted of the calculation of descriptive statistics and frequencies, significance testing with the Wilcoxon signed-rank test, and calculation of the Spearman’s rank correlation coefficient.
Long-term integrative psychotherapy program: Theoretical backgrounds, goals, and milestones
The suggested pattern of psychotherapy was developed on the basis of multi-theoretical psychotherapy (Brooks-Harris, 2008). We used an integrated cognitive and dynamic psychotherapy model applied to somatoform and anxiety disorders by Alla B. Kholmogorova and Natalya G. Garanian (1997, 2006). The model comprises various techniques: cognitive behavioral therapy and psychoanalytic therapy, as well as gestalt therapy and systemic family therapy.
In the psychotherapy considerable attention was paid to stimulating personality reflection, working on traumatic experiences, using personal problems and personality features to reveal inner resources, and extending the range of emotion-regulation strategies. The psychotherapy was undertaken within the theoretical framework of the cultural-historical concept developed by Lev S. Vygotsky. The following theses comprise the theoretical background of the study:
- Emotions as psychic phenomena can be attributed to the class of higher mental functions. Therefore, they reveal the following features: lifetime social development, mediated structure, and voluntary motivation in functioning (Vygotsky, 1935/1993, 1931/1997).
- The basic essentials of Vygotsky’s cultural-historical concept of mental development may be of theoretical value for psychosomatics and corporality psychology: human corporality may be interpreted as a cultural-historical phenomenon (Nikolaeva & Arina, 2003; Tkhostov, 2002).
- Personality reflection is regarded as a basis for self-regulation in accordance with key points of the concepts of Vygotsky, Aleksey N. Leontiev, and Bluma V. Zeigarnik (Vygotsky, 1935/1993, 1931/1997; Leontiev, 1978; Zeigarnik, 1972).
The main goals of the psychotherapy were as follows:
- to offer assistance to MVP patients in recognition of the psychological mechanisms in the clinical performance of the disease
- to provide training in emotion recognition, in mastering emotional states
- to extend the range of emotion-regulation strategies
- to stimulate personality reflection by working on traumatic experiences and on personality problems meant to reveal inner resources
- to work through the context of life and family problems
- to work through interpersonal problems
- to extend one’s repertory of coping processes
The psychotherapeutic program was provided in five stages:
1. Receiving information and motivation. This level embraced the following tasks:
- to bring about the operative (psychotherapeutic) alliance, confidence-building
- to inform patients of the connection between emotions and somatic symptoms and of the mental and somatic after-effects of the negligence of “emotional hygiene”; to reveal the “cultural conditionality” of neurotic disorders; to destroy the myth of the somatic nature of MVP and AD
- to present the model of psychotherapy, its tasks and methods
- to clarify the methods of self-regulation of psychological states and their aidless application in case of an emergency between treatment interviews (respiratory gymnastics, autogenic training); to demonstrate their efficiency in the treatment of anxiety fits
- to caution against the manifestation of counter-therapeutic factors in the process of treatment; their work-up: marking primary resistance
2.Receiving training in emotion recognition. This level had the following objectives:
- revealing problematic situations that cause negative emotions
- uncovering the difficulties patients can meet in marking, differentiating, and verbalizing emotions; these obstacles should be recognized as a psychotherapeutic problem
- shifting the presently adopted negative social mindset “it is unsafe to feel”
- distilling separate emotions within the complex inventory emerging in traumatic situations
3. Developing the skills of personality reflection and emotion regulation. This level required the following:
- revealing the interrelationship of emotions and thinking, on the one hand, and the interrelationship of emotions and vegetative reactions, on the other; encouraging shifting a dysfunctional mindset
- presenting the structural-dynamic model of emotion regulation
- presenting cognitive models of affective and somatic disorders
- leading the patient through the method of diary-keeping to register sensations, thoughts, and emotions that emerge in traumatic situations
- modulating emotiongenic situations during therapeutic meetings in order to name the experienced emotions, automatic thoughts, and somatic changes; empathically resolving anxiety; removing the inner ban on the expression of feelings and encouraging their open expression (“unfreezing”)
- analyzing “cognitive distortions”; providing training in methods of “cognitive mediation of emotions” to provide distance from dysfunctional thoughts (separating thinking and objective reality)
- developing “alternative logics”: turning one’s thoughts and emotions into the object of study, setting them within a broader system of relations and meanings, confronting them, relying on a new system of personal meanings
- working through personal resistance; discussing the “secondary gain” of disease
- detecting basic “distorted beliefs” and the primary formulation of personality problems, which become targets for further treatment
This stage meets increased resistance as patients face the imperative to change habitual ways of thinking and corresponding ways of behaving that are backed up by worldly philosophy. Another commonly recognized reason for resistance is patients’ improvement in general well-being, which contradicts the “secondary gain” of disease.
Therefore, it is important to warn patients of the difficulties they may encounter and to seek together for personality resources to negotiate them. It is important to inspire patients’ confidence in their ability to solve problems, to support and encourage them, and to help them find inner resources.
4. Analyzing previous experience, family context, and interpersonal relations.
At this stage the patient (together with the therapist) explores the inner sources of dysfunctional thinking and reveals personality problems. The analysis of family context takes into consideration the following: family myths, values, roles, rules, expectations, plans, and so on. Patients get a cathartic loosening of their traumatic experience. A survey of sources for basic beliefs and convictions is conducted. “Stereotypes of culture” are analyzed according to cultural-historical theory as an important source of beliefs and family myths. For example, the value of high-achievement motivation, typical for most patients, requires special attention.
5. Analyzing and working through personal problems; searching for resources for personality development. This level includes the following tasks:
- working on personal problems and looking for resources to resolve them
- setting urgent problems against a broader life context
- stimulating patients to shape alternative mindsets by relying on the analyzed consequences of negative beliefs, including shifting one’s view of oneself, of others, and of the world
- discussing the therapeutic effect achieved in the course of treatment; extending one’s repertory of coping processes and strategies of emotion regulation; broadening one’s range of psychological defense mechanisms, coping strategies, and strategies of emotion regulation, which provide for stress resistance and personal growth
Results
Analysis of the data obtained on the VAS, DISS, and PWB scales before and after therapy indicated that 78.1% of MVP patients demonstrated valid improvements of self-rated quality of life (QOL) after therapy and in the long term (Tables 2, 3, 4).
Table 2. Average values of well-being dimensions on the VAS in MVP patients with AD
Index |
Before therapy |
After therapy |
2-years Follow-up |
5-years Follow-up |
10-years Follow-up |
Well-being |
53.2±7.1 |
89.9±6.3** |
77.2±11.0* |
72.1±6.9* |
73.4±8.6* |
Note. ^Differences are significant when the data from the follow-up examinations are compared with the data of MVP patients examined before therapy (p<0.05). “Differences are significant when the data from the follow-up examinations are compared with the data of MVP patients examined before therapy (p<0.01).
Table 3. Average values of QOL indicators on the DISS in MVP patients with AD
Index |
Before therapy |
After therapy |
2-years Follow-up |
5-years Follow-up |
10-years Follow-up |
Work |
3.2 |
1.7* |
2* |
2.3 |
2.3 |
Social life dimension |
2.9 |
1.9* |
1.9* |
2.3 |
2.0* |
Personal life dimension |
2.6 |
1.7* |
1.9 |
2 |
1.9 |
Note. ^Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.05).
Table 4. Average values of well-being dimensions on the Ryff Scales of the PWB in MVP patients with AD
Areas of well-being |
Before therapy |
After therapy |
2-years Follow-up |
5-years Follow-up |
10-years Follow-up |
Self-acceptance |
42.82 |
72.38** |
59.18* |
53.32* |
55.84* |
Positive relations with others |
49.27 |
65.24 |
56.55* |
58.37* |
57.91 |
Autonomy |
40.00 |
57.45* |
52.76* |
49.09* |
52.12* |
Environmental mastery |
50.06 |
59.01* |
58.37 |
55.12 |
54.31 |
Purpose in life |
46.12 |
63.76* |
64.32* |
59.86* |
56.48* |
Personal growth |
47.72 |
66.83** |
67.14* |
61.38* |
52.14 |
Note. *Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.05). “Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.01).
Analysis of the dynamics in the emotional state of patients (before and after therapy and in the long term) with application of psychological dimensions revealed a tendency toward reduction of the anxiety level: trait anxiety indices went down from 49.0±6.1to 43.4±.3.5; state anxiety was reduced significantly from 47.1±5.9 to 39±3.8 on the Spielberger Scale (p<0.05). Processing of the follow-up data brought evidence that in two years the level of the mean-group indices of trait anxiety and state anxiety stayed within the range of moderate anxiety. In addition, the level of trait anxiety went down within two years of course completion. After both five and ten years, the level of anxiety was maintained within moderate range (Table 5).
Table 5. Average values of anxiety level on the Spielberger Scales in patients with MVP and AD
Index |
Before therapy |
After therapy |
2-years Follow-up |
5-years Follow-up |
10-years Follow-up |
Trait anxiety |
49.0±6.1 |
43.4±.3.5* |
38.1±6.4* |
45.3±4.9 |
42.9±4.2* |
State anxiety |
47.1±5.9 |
39±3.8* |
40.2±5.1* |
44.6±3.6 |
45.2±4.4 |
Note. *Differences are significant when the data from the follow-up examinations are compared with the data of MVP patients examined before therapy (p<0.05).
Analysis of the emotion-regulation strategies used by the patients before and after therapy showed that psychotherapy encouraged the use of strategies effective for solving adaptive tasks, such as:
- positive revision of the meaning of an event
- consecutive actualization of new meanings
- transformation of an experience through the use of humor
- change in the expressive characteristics of emotions with transforming catharsis
As a result, such strategies as rumination and catastrophization, comparison and devaluation of the meaning of events and personal experience, and direct catharsis and repression of emotions grew increasingly rare (Table 6).
Table 6. Strategies of emotion regulation in MVP patients with AD (frequency analysis, %)
No. |
Strategies of emotion regulation |
Before therapy |
After therapy |
2-years Follow-up |
5-years Follow-up |
10-years Follow-up |
1. |
No changes in answer when the instruction has been changed |
26.8 |
6.3** |
10.1** |
9.9** |
9.2** |
2. |
Cognitive changes: total |
73.2 |
93.7* |
89.9 |
90.1 |
90.8 |
2.1. |
Ruminations and catastrophization |
19.6 |
12.1* |
11.3* |
12.6 |
16.9 |
2.2. |
Comparison and devaluation |
26.5 |
20.5 |
14.4* |
11.1** |
17.8* |
2.3. |
Positive revision |
8.3 |
11.0 |
10.4 |
15.8* |
16.8** |
2.4. |
Consecutive actualization of new meanings |
18.8 |
40.5** |
39.5** |
35.3* |
31.4* |
2.5. |
Transformation of experiences through the use of humor |
0 |
9.6** |
14.3** |
15.3** |
7..9** |
3. |
Change in the expressive Characteristics of emotions: total |
100 |
100 |
100 |
100 |
100 |
3.1. |
Direct catharsis |
27.6 |
12.7** |
15.3* |
16.9* |
16.2* |
3.2. |
Repression of emotions |
31.9 |
20.3* |
15.6** |
18.9* |
25.3* |
3.3. |
Communicative catharsis |
23.8 |
26.8 |
26.9 |
27.3* |
23.8 |
3.4. |
Transforming catharsis |
16.7 |
40.2** |
42.2** |
36.9** |
34.7** |
Note. *Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examination before therapy (p<0.05). “Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.001).
Psychiatric diagnostics revealed a significant (p<0.05) reduction in the frequency and intensity of panic attacks and in anticipatory anxiety of panic attacks (PA); the frequency and intensity of phobias went down, and there was a considerable decline in the avoidance of phobic situations (Table 7).
Table 7. Frequency and intensity of PA and phobias and frequency of avoidance of phobic situations in MVP patients with AD (points, M±m)
Indices |
Before therapy |
After therapy |
2-years Follow-up |
5-years Follow-up |
10-years Follow-up |
Frequency of severe situational PA (per week) |
0.4±0.1 |
0.1±0.08** |
0.2±0.09* |
0.2±0.06* |
0.3±0.03 |
Intensity (points) |
1.4±0.3 |
0.7±0.,3* |
0.6±0.2* |
0.9±0.1 |
1.0±0.1 |
Frequency of severe spontaneous PA (per week) |
0.5±0.2 |
0.08±0.02** |
0.2±0.09* |
0.3±0.09 |
0.3±0.08 |
Intensity (points) |
1.8±0.5 |
0.6±0.3** |
1.0±0.6** |
1.3±0.09 |
1.5±0.06* |
Frequency of light situational PA (per week) |
0.9±0.1 |
0.2±0.07** |
0.7±0.2 |
0.6±0.09 |
0.9±0.2 |
Intensity (points) |
1.5±0,4 |
0.5±0,2* |
1.1±0.4 |
1.0±0.2 |
1.4±0.4 |
Frequency of light spontaneous PA (per week) |
2.9±0,1 |
0.8±0,1* |
1.6±0.09* |
2.0±0.1* |
1.9±0.3 |
Intensity (points) |
4.7±0,5 |
0.5±0,2** |
3.3±0.4* |
4.0±0.4* |
4.1±0.4* |
Anxiety caused by expectation of PA (points) |
4.6±1.9 |
1.2±0.4** |
2.1±0.6** |
2.5±0.5* |
2.9±0.7* |
Phobias (points) |
1.2±0.4 |
0.5±0.2* |
0.7±0.09* |
0.9±0.09 |
1.0±0.1 |
Avoidance of phobic situations (points) |
0.7±0.4 |
0.3±0.5* |
0.4±0.1* |
0.5±0.07 |
0.6±0.09 |
Note. *Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.05). “Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.01).
After therapy there was a significant decrease in the severity of dysautonomic symptoms. The number of patients with severe dysautonomic symptoms dropped more than 4.5 times. The follow-up study showed relative retention of this therapeutic effect (Table 8).
Table 8. Intensity of dysautonomic symptoms in MVP patients with AD (frequency analysis, %)
|
Before therapy |
After therapy |
2-years Follow-up |
5-years Follow-up |
10-years Follow-up |
Severe dysautonomia |
71.9 |
9.4** |
9.4** |
12.5** |
17.9** |
Moderate dysautonomia |
18.7 |
46.9** |
53.2** |
50.0** |
57.1** |
Light dysautonomia |
9.4 |
37.4** |
37.4** |
31.2** |
17.9* |
Absence |
- |
6.3** |
0 |
6.3** |
7.1** |
Note. *Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.01). “Differences are significant when the data from the follow-up studies are compared with the data of MVP patients examined before therapy (p<0.001).
Physical examination of the patients revealed a significant (p<0.05) reduction in the frequency and intensity of chest pain (especially pain provoked by emotions), in psychogenic gastrointestinal disorders, in loops of thermal control, and in neurogenic hyperventilation syndrome. The differences are significant when we compare results of the survey before and after therapy and 2, 5, and 10 years after the completion of therapy (Figure 1).
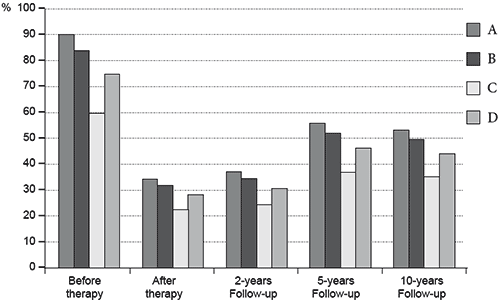
Figure 1. Intensity of dysautonomic symptoms in patients with MVP before and after therapy and in the follow-up study. А: chest pain; В: psychogenic gastrointestinal disorders; С: loops of thermal control; D: neurogenic hyperventilation syndrome.
Psychotherapy encouraged reductions in the frequency of a considerable number of analyzed vascular disorders and, to a considerable extent, in the frequency of tension-type headaches; differences are highly significant (p<0.001) when we compare the results of the survey before and after therapy and 2 years after the completion of therapy, and the differences are reliable 5 and 10 years after the end of psychotherapy (p<0.05) (Figure 2).
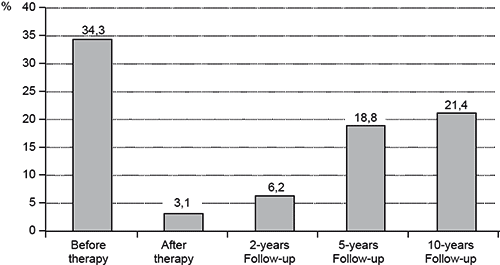
Figure 2. Frequency of tension-type headaches in MVP patients before and after therapy and in the follow-up study
An estimate of the psychiatric index of therapeutic efficacy was carried out on the Clinical Global Impression scale. It revealed significant efficacy for 78.6% of the patients, a medium index for 14.3 %, and a minimum index for 7.1%. Clinically significant efficacy of therapy for general symptomatic relief was reported for 73.7% of the patients. The follow-up study showed that high indices of the achieved therapeutic effect were retained for 2 to 3 years after the course of therapy. After that time frame, patients usually resorted to psychological care whenever they were caught in emotiogenic situations.
The control group did not reveal any increase in psychological and physical indices during 15 years.
Thirty-two MVP patients who volunteered for the course of individual integrative psychotherapy provided results for the follow-up study.
Remote catamnesis data revealed the following:
- 81.3% of the patients had a stable job after the course of psychotherapy.
- 75% of interviewed patients were reported by the psychiatrist to be in sustained remission.
- 78.1% of the interviewed patients reported positive dynamics in their family relations (marriage, childbirth, conflict avoidance, and stability of family life) for a long period of time; the achievements were associated with the positive impact of the therapy.
- 68.8% of the interviewed patients described their state of physical health as good; 31.2% of the patients believed it to be satisfactory.
- 68.8% of the interviewed patients described their current psychological state of health as good, 6 patients (18.8%) described it as satisfactory, and 3 people (9.4%) described it as bad.
- 93.8% of patients showed an increase in frustration tolerance.
- Most of the patients associated all positive changes with the course of psychotherapy.
Thus 23 people (71.9% of those interviewed) described the psychotherapy as having a considerable effect, 7 patients (21.9%) assessed it as having a moderate effect, and only 2 people (6.3%) denied any positive effect of the therapy.
Discussion
Results of the study may be summed up as follows: MVP patients with AD who attended courses of long-term psychotherapy showed definite improvement in both psychological and clinical features. They experienced a considerable decrease in their level of anxiety, and the indices of well-being were higher after the courses of therapy than before. As for emotional regulation, the patients revealed a considerable increase in the use of effective and complicated cognitive strategies, such as positively revising the meaning of an event, consecutively actualizing new meanings, and transforming an experience through the use of humor. In addition, such strategies as rumination and catastrophization, comparison and devaluation of the meaning of events and personal experience, direct catharsis and repression of emotions grew increasingly rare.
Discovered changes in the conceptualization of traumatic events and the selection of strategies for emotion regulation vividly testify to increased personality reflection and ability to regulate emotions and to growing awareness of actual needs, individual purposes, and resources of personality. Positive dynamics in the development of personality reflection, recognition of emotional experience with improved skills of self-regulation, and growing awareness of actual needs, individual purposes, and resources of personality were associated with positive dynamics in clinical symptoms. Psychiatric diagnostics revealed a reduction in the frequency and intensity of panic attacks, in the anticipatory anxiety of panic attacks, and in the frequency and intensity of phobias, and also a considerable decline in the avoidance of phobic situations. Most of the interviewed patients were reported by the psychiatrist to be in sustained remission.
The follow-up study showed that high indices on the achieved therapeutic effect were retained for 2 to 3 years after the course of therapy; relative retention of therapeutic effect was also reported in reexamination after 5 and after 10 years. When compared, the data of psychological and clinical follow-up examinations of MVP patients with AD who attended the courses of long-term psychotherapy and the data of those patients who refused to attend the courses or who undertook only short-term psychotherapy reveal evidence of positive dynamics in patients’ psychological features and in their patterns of disease after the long-term psychotherapy. These dynamics include an increase in well-being dimensions and personality reflection, an extension of the repertoire of emotion-regulation strategies and coping strategies, and a reduction in anxiety and clinical presentations of MVP in the group of patients attending the courses of psychotherapy (Pervichko, Zinchenko, & Martynov, 2013; Zinchenko, Pervichko, & Martynov, 2013 a, 2013b).
Results of the study are in accordance with the data presented in the scientific works of Stavrakaki, Gonzalez, and others. They describe cases of genuine reduction in the intensity of clinical symptoms in MVP patients after psychotherapy and antidepressant or anxiolytic treatment (Gonzalez et al., 2002; Pariser et al., 1981; Scordo, 2007; Stavrakaki et al., 1991).
The results lead us to the conclusion that features of anxiety disorders displayed by MVP patients in combination with disorders of personality reflection and emotion regulation may be regarded as “psychological risk factors” that aggravate the clinical symptoms of MVP. An increase in clinical MVP presentations appears mostly in emotionally loaded situations when no medication and psychological treatment is provided (Zinchenko & Pervichko, 2012, 2014).
The data suggest an urgent necessity to extend the medical treatment of MVP patients with long-term psychotherapy. The results make way for new strategies of psychotherapy for MVP patients with AD. The results were obtained through application of the theoretical and methodological principles of Vygotsky’s cultural- historical theory and the principles of the Vygotsky-Luria concept of syndrome analysis (Vygotsky, 1935/1993; Luria, 1973).
Conclusions
MVP patients with AD who attended courses of long-term psychotherapy showed distinct improvement in both psychological and clinical features. Positive dynamics of clinical symptoms were associated with the development of personality reflection, recognition of emotional experience, improved skills of self-regulation, and growing awareness of actual needs, individual purposes, and resources of personality.
The results suggest an urgent necessity to extend the medical treatment of MVP patients with long-term psychotherapy aimed at stimulating personality reflection, working on traumatic experience, and working on personal problems and personality features in order to reveal inner resources and to extend the range of emotion- regulation strategies.
References
Barlett, C. C., Kirtley, M., & Mangham, R. (1991). Mitral valve prolapse. Journal of the Louisiana State Medical Society, 143(5), 41-43.
Brooks-Harris, J. E. (2008). Integrative multitheoretical psychotherapy. Boston: Houghton Mifflin.
Coplan, J. D., Papp, L. A., King, D. L., & Gorman, J. M. (1992). Amelioration of mitral valve prolapse after treatment for panic disorder. American Journal of Psychiatry, 149(11), 15871588.
Devereux, R. B., Kramer-Fox, R., & Kligfield, P. (1989). Mitral valve prolapse: Causes, clinical manifestations, and management. Annals of Internal Medicine, 3(4), 305-317. doi:10.7326/0003-4819-111-4-305
Gonzalez, E. A., Pimentel, C., Natale, R. A., Toll, B. A., Soffer, A., & Gralnik, L. M. (2002). Psychiatric and medical comorbidity in mitral valve prolapse. Irish Journal of Psychological Medicine, 19(1), 16-20.
Gorman, J. M., Goetz, R. R., Fyer, M., King, D. L., Fyer, A. J., Liebowitz, M. R., & Klein, D. F. (1988). The mitral valve prolapse-panic disorder connection. Psychosomatic Medicine, 50(2), 114-122. doi:10.1097/00006842-198803000-00002
Guy, W. (Ed.). (1976). ECDEU Assessment Manual for Psychopharmacology. Rockville, MD: Alcohol, Drug Abuse, and Mental Health Administration, Public Health Service, U.S. Department of Health, Education, and Welfare.
Joiner, C. R., & Cornman C. R. (1986). The mitral valve prolapse syndrome: Clinical features and management. Cardiovascular Clinics, 10(2), 233-256.
Kholmogorova, A. B., & Garanian N. G. (1997). Integration of cognitive and psychodynamic approaches in the psychotherapy of somatoform disorders. Journal of Russian and East European Psychology, 35(6), 29-54. doi:10.2753/RP01061-0405350629
Kholmogorova, A. B., & Garanian, N. G. (2006). Psychological care to individuals with traumatic stress experience. Moscow: UNESCO, MGPPU.
Leontiev, A. N. (1978). Activity, consciousness, and personality. Englewood Cliffs, NJ: Prentice Hall.
Luria, A. R. (1973). The working brain: An introduction to neuropsychology. London: Penguin Books.
Nikolaeva, V. V., & Arina, A. G. (2003). Kliniko-psihologicheskie problemy psihologii telesnosti [Clinical and psychological problems in corporeality psychology]. Psihologicheskij Zhurnal [Psychological Journal], 24(1), 119-126.
Pariser, S. F., Reynolds, J. C., Falko, J. M., Jones, B. A., & Mencer, D. L. (1981). Arrhythmia induced by a tricyclic antidepressant in a patient with undiagnosed mitral valve prolapse. American Journal of Psychiatry, 138 (4), 522-523.
Pervichko, E., Zinchenko, Yu., & Martynov, A. (2013). Peculiarities of emotional regulation with MVP patients: A study of the effects of rational-emotive therapy. Procedia—Social and Behavioral Sciences, 78, 290-294. doi:10.1016/j.sbspro.2013.04.297
Rosenzweig, S. (1978). The Rosenzweig Picture Frustration (P-F) Study: Basic manual. Odessa, FL: Psychological Assessment Resources.
Ryff, C. (1989). Happiness is everything, or is it? Explorations on the meaning of psychological well-being. Journal of Personality and Social Psychology, 57, 1069-1081. doi:10.1037/00223514.57.6.1069
Ryff, C., & Keyes, C. (1995). The structure of psychological well-being revisited. Journal of Personality and Social Psychology, 69, 719-727. doi:10.1037/0022-3514.69.4.719
Scordo, K. (2007). Medication use and symptoms in individuals with mitral valve prolapse syndrome. Clinical Nursing Research, 16, 58-71. doi:10.1177/1054773806295240
Sheehan, D. V. (1983). The Anxiety Disease. New York: Scribner.
Sheehan, D. V., & Harnett-Sheehan, K. (1990). Psychometric assessment of anxiety disorders. In N. Sartorius, V. Andreoli, G. Cassano, L. Eisenberg, P. Kielholz, P. Pancheri, & G. Racagni (Eds.), Anxiety: Psychobiological and clinical perspectives (pp. 85-100). New York: Hemisphere.
Spielberger, C. D., Gorsuch, R. L., Lushene, R., Vagg, P. R., & Jacobs, G. A. (1983). Manual for the State-Trait Anxiety Inventory. Palo Alto, CA: Consulting Psychologists Press.
Stavrakaki, C., Williams, E., Boisjoli, A., Vlad, P., & Chasse, H. (1991). Mitral valve prolapse and psychiatric complications: A case report. Journal of Psychiatry and Neuroscience, 16(1), 45-49.
Stefanadis, C., & Toutouzas, P. (2000). Mitral valve prolapse: The merchant of Venice or much ado about nothing? European Heart Journal, 2, 255-258. doi:10.1053/euhj.1999.1926
Tkhostov, A. S. (2002). Psihologija telesnosti [Corporality psychology]. Moscow: Smysl.
Vygotsky, L. S. (1993). The diagnostics of development and the pedological clinic for difficult children. In R. W. Rieber & A. S. Carton (Eds.), The collected works of L. S. Vygotsky: The fundamentals of defectology (abnormal psychology and learning disabilities), 2, 241-291. New York: Plenum. doi:10.1007/978-1-4615-2806-7. (Original work published 1935)
Vygotsky, L. S. (1997). Genesis of higher mental functions. In R. W. Rieber & A. S. Carton (Eds.), The collected works of L. S. Vygotsky: The history of the development of the higher mental functions, 4, 97-120. New York: Plenum. doi:10.1007/978-1-4615-5939-9 (Original work published 1931)
Zeigarnik, B. V. (1972). Experimental abnormal psychology. New York: Plenum. doi:10.1007/9781-4684-7421-3
Zinchenko, Yu. P., & Pervichko, E. I. (2012). The methodology of syndrome analysis within the paradigm of “qualitative research” in clinical psychology. Psychology in Russia: State of the Art, 5, 157-184. doi:10.11621/pir.2012.0010
Zinchenko, Yu. P., & Pervichko, E. I. (2014). Heuristic value of post-non-classical models in psychosomatics (on the example of L. S. Vygotsky and A. R. Luria’s syndrome approach). Voprosy Psykhologii [Issues in psychology], 1, 14-27.
Zinchenko, Yu. P., Pervichko, E. I., & Martynov, A. I. (2013a). Emotional experiences and coping processes in the context of verification of psychosomatic hypotheses in MVP patients. Procedia—Social and Behavioral Sciences, 86, 47-52. doi:10.1016/j.sbspro.2013.08.523
Zinchenko, Yu. P., Pervichko, E. I., & Martynov, A. I. (2013b). Psychological underpinning of personalized approaches in modern medicine: Syndrome analysis of mitral valve prolapse patients. Psychology in Russia: State of the Art, 6(2), 89-102. doi:10.11621/pir.2013.0208
To cite this article: Zinchenko Y., Pervichko E., Akatova E. (2014). Dynamics of the psychological features and clinical symptoms in mitral valve prolapse patients receiving long-term integrative psychotherapy for anxiety disorders. Psychology in Russia: State of the Art, 7(3), .
The journal content is licensed with CC BY-NC “Attribution-NonCommercial” Creative Commons license.










